Last Updated on March 4, 2024
This guide provides useful information that will help with your decision to become a Navy Medical Corps Officer during Fiscal Year 2024.
A Medical Corps Officer is a Staff Corps Officer in the Navy who provides care to military members and their families in the same manner that a civilian doctor would. The Navy Officer designator code for Medical Corp Officer is 2100.
As you will see, there are many specialties within the Medical Corps. Each will have their own special requirements.
We will discuss these in detail, but let us start with the basics.
Medical Corps Officer Job Description
As mentioned, as a Navy Medical Corps physician, you will treat servicemembers and their families in the same manner that a civilian doctor would.
However, in the realm of Navy Health Care, you will get a larger range of expertise quicker since you will be practicing at the cutting edge of medicine.
When you join the Navy as a doctor and Medical Officer, you will advance your career well ahead of your contemporaries, with the option to participate in humanitarian assistance activities both at home and throughout the globe.
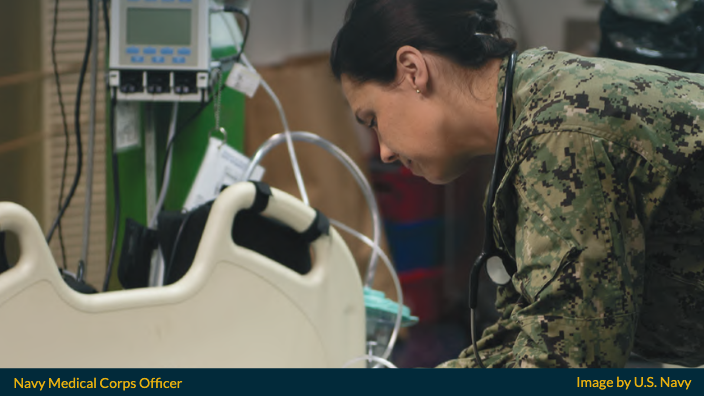
Working at top military medical institutions gives you access to sophisticated training and technology that is so advanced that the civilian world may not be aware of it yet.
Navy doctors often use adjectives like “amazing” and “the best” to praise their patients and medical staff.
You, like them, will acquire a unique feeling of camaraderie and will be able to concentrate on the finer parts of medicine without the financial and economic problems that come with private practice.
As a Navy Physician, you will play an important role in leading the well regarded Navy Health Care staff.
You can help with medical relief operations in our nation and throughout the world, helping victims of anything from illness to conflict, disease to poverty, and hurricanes to earthquakes.
You will use cutting-edge technology like Light-Emitting Diode (LED) probes created in collaboration with NASA to help wounds heal quicker.
Not only that, but you will also get to experience cutting-edge techniques like “forward surgery,” which connects field medics with bigger medical centers for life-saving advice and treatment.
Aside from that, you will:
- Distinguish yourself as a Navy Physician and Medical Corps Officer with pride and respect
- Experience manageable patient ratios for high-quality, one-on-one care
- Earn excellent compensation in an established, thriving practice
- Expand your expertise through hands-on experience and Navy-funded advanced training
When you practice Navy Medicine, you will not have to deal with many of the challenges that your civilian counterparts may face:
- No malpractice insurance to purchase
- No employees to recruit
- No startup expenditures
- No equipment to purchase
- No office to furnish
You will also have a more flexible schedule, which means more time for family, personal interests, and adventure.
Responsibilities of Navy Physicians
As a Navy Medical Corps Officer, you will deliver high-quality medical treatment to Sailors, Marines, servicemembers, their families, and, when called upon, any individual worldwide.
You will be in charge of everything a conventional physician does, such as diagnosing illnesses, treating injuries, and saving lives.
Then you will have the chance to go beyond the mundane:
- Acquire managerial experience that will help you throughout your career
- Collaborate with fellow military doctors and other Health Care Officers, and partner with International Relief Teams and organizations such as FEMA and USAID
- Operate as a leader within your focus area, while also gaining exposure outside your specialty
- Work at the best military medical facilities on land, at sea, and even in the battlefield
What to Expect as a Navy Physician
As a member of the Navy Medical Corps, you may serve at any of the more than 250 Navy and medical institutions throughout the world, in some of the most dynamic settings conceivable – from Hawaii to Japan, Germany to Guam, and Washington, D.C. to Washington state.
You may work in one of the highly regarded Medical Centers in Bethesda, Maryland, Portsmouth, Virginia, or San Diego, California.
Alternatively, you might give medical assistance to deployed soldiers aboard one of two specialist hospital ships, the USNS Comfort and USNS Mercy.
The Navy Medical Corps is made up of about 4,300 active duty and reserve doctors who work or train in 23 medical and surgical specialties, with over 200 subspecialties.
Navy doctors work at military treatment facilities, medical education institutes, clinics, hospitals, research units, aboard ships, and with Marine Forces in the United States and across the world.
Navy doctors offer direct assistance to commanders, squadrons, battalions, and units of the Navy and Marine Corps.
Furthermore, Navy physicians deploy to support combat operations, disaster relief, and humanitarian aid missions, offering the finest treatment our country has to offer both on land and at sea.
More health-care options are available both at home and overseas in a variety of contexts, including on board a surface ship, collaborating with a neighboring aviation squadron, or even the Fleet Marine Force. Whatever position you hold, you will contribute leadership and knowledge to your nation, the men and women who protect it, their families, and those in need.
Navy Medicine
Navy Health Care is genuinely world-class when it comes to health-care networks.
A devoted organization of thousands of doctors, dentists, nurses, and healthcare specialists working together to serve the public.
They support the many needs of servicemembers, their families, and mankind as a whole, spreading kindness and wellness wherever it is needed.
Whether it is saving lives or promoting good health, reaching out to those in need or driving the field of healthcare ahead, Navy Health Care offers a chance unlike any other.
To be a part of anything significant.
To be a part of a world-class health-care team that makes an impact on a global scale.
And to experience challenges and rewards that are normally unavailable in the private sector.
Navy Medical Corps Specialties
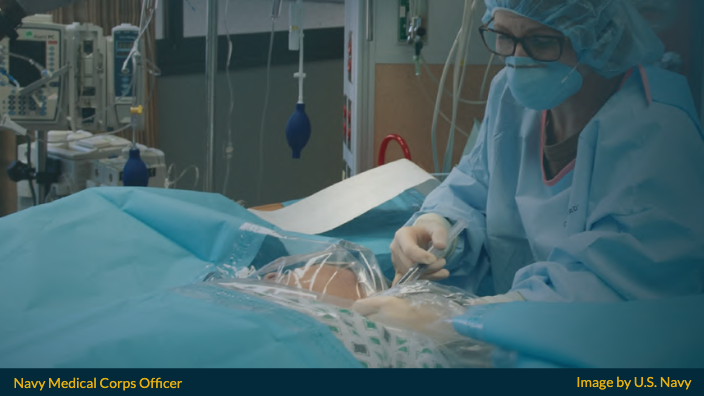
Navy Medicine provides clinical practice opportunities in over 30 specialties and subspecialties, including:
- Anesthesiology
- Dermatology
- Emergency Medicine
- Family Medicine
- Fleet Marine Corps Medicine
- Geriatrics
- Global Health Engagement
- Internal Medicine
- Allergy/Immunology
- Cardiology
- Endocrinology
- Gastroenterology
- Hematology/Oncology
- Infectious Disease
- Nephrology
- Pulmonary/Critical Care
- Rheumatology
- Histopathology
- Neonatology
- Neurology
- Nuclear Medicine
- Obstetrics/Gynecology
- Occupational Medicine
- Ophthalmology
- Orthopedics
- Osteopathic Medicine
- Otolaryngology
- Pain Management
- Pathology
- Pediatrics
- Physical Medicine
- Plastic and Reconstructive Surgery
- Preventive Medicine
- Psychiatry
- Transfusion Medicine
- Tropical Medicine
- Undersea/Diving Medicine
- Urology
Operational Medical Officer
The Navy is unusual among military forces in that doctors work in all realms of battle – land, sea, air, space, and cyberspace.
Throughout your career, you will have the chance to work with individuals in all of these environments.
In the Navy, you will practice medicine in a variety of settings, including:
- In conventional hospitals and clinics (otherwise called Military Treatment Facilities or MTFs)
- Units and field hospitals (for example, an Expeditionary Medical Facility)
- On board ships (Surface Force Medicine)
- Submerged (Undersea Medicine)
- In the Sky (Aviation Medicine)
- As a member of the United States Marine Corps (Fleet Marine Force Medicine)
- General Medical Officers, or GMOs, have traditionally provided operational medical care. These are doctors who have finished their internship but have deferred their residency study in order to serve the fleet.
For a variety of reasons, Navy Medicine is shifting from an interrupted training system to one of continuous training, in which medical students will complete their residency training in a straight-through/uninterrupted manner, in accordance with the civilian timetable.
As a consequence, Navy Medicine will most likely have fewer GMOs and will place more residency-trained doctors in operational settings.
These residency-trained doctors are known as Operational Medical Officers (OMO).
It will be a slow shift, and some GMOs will be required even when the change is complete.
This will appeal to anybody who does not want to finish their residency linearly.
The descriptions of each operating community accessible to you in Navy Medicine are listed below.
Undersea Medical Officer
Undersea Medical Officers (UMOs) are doctors who have received specialized training in the physiological strains of hyperbaric and hypobaric conditions, as well as exposure to low-level ionizing radiation, atmospheric control concerns, and lengthy durations in isolated locations.
Previously, most doctors became UMOs after completing an internship.
With the move to OMOs, more residents are anticipated to begin training after their residency usage tour.
With 108 billets (military terms for posts or occupations), the UMO community plays an important role within the Submarine Force, Naval Special Warfare, Marines, Diving Units, and Research communities.
UMOs are specialists in Dive Medicine, Submarine Medicine, and Radiation Health, and they offer healthcare to people who operate in the underwater environment.
They uphold particular duty requirements while also training and supervising Independent Duty Corpsmen.
They also provide medical advice to top commanders and are an important component of these unique societies.
Submarine squadrons and groups, Naval Special Warfare, Explosive Ordnance Disposal, Marine Special Operations (MARSOC), Navy Diving Commands, Naval Reactor Prototypes, Research Labs, MTFs, clinics, training institutes, and many other sites use UMOs.
UMOs have special physical requirements due to the diving experience required in this area and must fulfill the minimum Diver Physical Criteria Test standards.
In Groton, CT, UMO training starts with 6 weeks of physical fitness, radiation health, and submarine medicine.
After that, UMO trainees move to Panama City, FL, for 9 weeks of dive/hyperbaric medicine, open circuit SCUBA training, surface supplied diving, closed circuit SCUBA, and hyperbaric chamber operations.
UMOs who complete this training are certified as Navy Divers.
After that, UMO students return to Groton, CT, to finish their training with 8 weeks of damage control/submarine escape, clinical hyperbaric oxygen treatment, operational medicine, and a full oral board test.
Aviation Medicine
Aviation Medicine is a specialization that considers the aviator’s unique and demanding environment while making medical decisions and treating them.
It is a chance to work directly in support of the Sailors and Marines protecting our country in a highly customized and intimate setting.
As a Flight Surgeon, you will likely be assigned to an aircraft squadron or to a command that oversees many squadrons.
They will see you as their personal physician, fellow aviator, and often friend, a unique and treasured connection.
These trips give possibilities for fresh and unusual experiences, travel, and autonomy in operating your medical practice.
These experiences will provide you with the leadership, initiative, self-assurance, planning ability, foresight, teaching ability, and organizational abilities expected of doctors working with operational forces.
A Flight Surgeon’s responsibilities include practicing preventive medicine by assuring safety in the air and workplace, promoting aviation safety by lowering the risk of aviation catastrophes by bridging the gap between the practice of medicine, the science of safety, and the profession of aviation.
Flight surgeons evaluate the squadron and aircraft environments by flying as aircrew with the squadron and observing in-flight stresses and crew cohesion.
The Flight Surgeon curriculum is a 26-week training course that includes flight physiology, industrial hygiene/occupational medicine, environmental hazards, and aviation accident investigations.
Training courses are held three times a year, and graduates are required to exercise in an operational scenario to guarantee an aircraft unit is battle ready.
Phase I consists of the first seven weeks of academics and aquatic survival training, followed by environmental physiology, naval aviation medicine, operational medicine, and aerospace ENT/Ophthalmology/Psychiatry/Internal Medicine/Neurology.
Phase II consists of a 6-week Aviation Preflight Indoctrination (API) and Ground School program.
Acquainting yourself with the aviation community Aerodynamics, engines and systems, navigation, weather, basic water survival, and aviation physiology are among the topics taught.
Phase III is an 11-week flight indoctrination course that introduces students to the risks and pressures of flying from the viewpoint of aviators.
The remaining two weeks are dedicated to learning about the Naval Aviation Safety Program and how you may become a part of it.
As you will often be the sole and best resource for the human element assessment, a section of this course will concentrate on aviation crash investigation.
Aside from the physical standards, flight surgeons must also fulfill the anthropometric specifications required by aviation schools.
These criteria are quite flexible, and exemptions are possible.
More than 240 flight surgeon billets are available in the Navy and Marine Corps, including in Italy, Bahrain, Japan, Diego Garcia, and across Hawaii and the United States.
Other similar occupations include Aviation Medical Examiner, which needs 7 weeks of academic instruction in aviation medicine but does not entail flying training.
These roles are primarily concerned with clinical aviation medical assistance, with little flying time or prolonged physical needs.
The Navy Residency in Aerospace Medicine is a two-year program that educates medical officers for board certification in Aerospace Medicine via an emphasis on preventative and occupational medicine.
Aerospace Medicine professionals are expected to be thought leaders in aerospace and preventative medicine, with experience in operational and MTF contexts.
Surface Force Medical Officer
Surface Force Medical billets are critical operational leadership possibilities for any Medical Officer who chooses to serve on board or in support of Surface Force ships.
Medical Corps Officers are required to be medical subject-matter experts, department heads, and special aides to the Commanding Officers in these posts, which necessitates leadership experience.
There are chances on a broad range of ships and at a number of places across the globe.
There is an expectation that you will be able to give information in a variety of areas, such as industrial hygiene, occupational medicine, preventive medicine, emergency medicine, medical evacuation, and medical intelligence.
As the ship’s Department Head, you will be in charge of all medical concerns for the crew, departmental organization and training, medical correspondence, staff assignments and watches, personnel performance assessments, and guaranteeing promotion preparedness for your team.

Fleet Marine Medical Officer
Fleet Marine Medical Officers (FMMOs) provide medical advice to Marine Corps Commanding Officers.
They are in charge of medical readiness and the supervision of Independent Duty Corpsmen, physician assistants, and Hospital Corpsmen.
They offer patient care, patient tracing, and emergency trauma treatment and resuscitation in the field.
Likewise, they serve as the Medical Department Head and are supposed to behave like a Marine, knowing Marine Corps history and customs, shooting, running, hiking, and looking the part.
They also must fulfill Fleet Marine Force (FMF) Qualification criteria and act as role models for their peers and enlisted soldiers.
Officership 101, Field Medical Training Battalion-Field Medical Service Officer, Tactical Combat Casualty Care (TCCC), Fresh Whole Blood Transfusion, Basic Rifle Marksmanship, and USMC Customs and Courtesies are among the subjects covered in Marine Corps training.
Navy Medical School Scholarships and Incentives
With extensive financial support and continuing education programs, the Navy can help reduce your financial responsibilities and develop your profession, no matter where you are in your medical career.
Scholarships, sign-on incentives, and debt repayment aid are examples of available options. And assistance may be available whether you are in graduate school, residency, or already in practice.
Health Professional Scholarship Program (HPSP)
The Health Professions Scholarship Program (HPSP) provides a full-tuition scholarship to the medical school of your choice, as well as a monthly stipend surpassing $2,300 per month and a $20,000 signing bonus in exchange for a three or four-year commitment to service as a Navy physician following residency.
Here is the official document for HPSP.
Health Services Collegiate Program (HSCP)
In exchange for duty as a Navy physician following residency, this program gives up to $269,000 while attending medical school, including a monthly military wage, considerable housing allowance (depending on location), and a full benefits package.
Here is the official document for HSCP.
Direct Commissioning
Practicing medical doctors may receive a sign-on bonus of $180K to $400K when you qualify. Incentive offers have many variables depending on the service agreement and chosen specialty.
Here is the official document for Medical Corps commissioning.
Uniformed Services University of the Health Sciences (USU)
Individuals may also apply to the Uniformed Services University of Health Sciences directly.
Students who are approved get free tuition, a housing allowance, and a wage.
As “America’s Medical School,” USU educates, trains, and comprehensively prepares uniformed military and United States Public Health Service physicians to support our nation’s military and public health systems, the United States’ National Security and National Defense Strategies, and the readiness of our Uniformed Services.
Here is the admission information at USU.
Financial Assistance Program (FAP)
The Financial Assistance Program (FAP) offers financial incentives to doctors who complete certain residencies and fellowships that lead to postings on active service in the Medical Corps.
While completing your residency or fellowship, you will be eligible for a $45,000 yearly award and receive a monthly compensation of more than $2,300.
Navy Physician Basic Qualification
To become a Navy Medical Corps Officer, you must be an American citizen no older than 42 years of age with a qualifying medical degree and license as prescribed by the United States Navy. Qualified students who are admitted to an accredited medical school may apply for a Navy Medical Corps scholarship.
The detailed list of Medical Corps Officer requirements below are current as of July 2019, per the Navy Personnel Command. No updates have been issued so far.
Medical Corps Officer Basic Qualifications
Citizenship
Unless waived by the Secretary of Defense for an original appointment at a grade lower than lieutenant commander, U.S. citizenship is necessary (born in the United States, naturalized, or born abroad of U.S. parents) to apply for the Medical Corps Officer program.
Dual citizens are able to apply, but they must provide documentation of renunciation of non-U.S. citizenship before being considered for final selection.
SECNAVINST 5510.30B (Department of the Navy (DON) Personnel Security Program (PSP) Instruction) requires a personnel security investigation for all applicants.
Age
Applicants for the Medical Corps must be commissioned before their 42nd birthday.
Waivers will be handled on an individual basis.
Age Waiver
An age waiver may be approved in restricted numbers in circumstances when the candidate exceeds the statutory age for commissioning but otherwise has an extraordinary record or demonstrated expertise needed by the Navy.
When evaluating age waiver requests, a heavy focus will be placed on undermanned specialities and those with a history of unmet recruiting targets.
Gender
The Medical Corps Officer program is open to both men and women with no restrictions.
Education
To be qualified for appointment in the Navy Medical Corps, the candidate must complete one of the following educational qualifications, as outlined in OPNAVINST 1120.4C (Appointment of Regular and Reserve Officers in the Medical Corps of the Navy):
- Physician (Doctor of Medicine): Graduate of a medical school in the United States or Puerto Rico approved by the American Medical Association’s Liaison Committee on Medical Education and licensed to practice medicine or surgery in a U.S. State, territory, commonwealth, possession, or the District of Columbia.
- Physician (Doctor of Osteopathy): Graduate of an American Osteopathic Association-approved institution of osteopathy and be licensed to practice medicine, surgery, or osteopathy in a U.S. State, territory, commonwealth, possession, or the District of Columbia.
- Physician graduates of foreign medical schools in specialties approved by the Deputy Chief Of Naval Operations (Manpower, Personnel, Training and Education) who complete all standards stipulated in OPNAVINST I 120.4C.
Physical
Medical Corps applicants must meet physical standards in accordance with Chapter 15, Manual of the Medical Department and as specified in DoD Instruction 6130.03 dated May 6, 2018, (Medical Standards for Appointment, Enlistment, Or Induction in the Military Services).
Licensure
Applicants for the Medical Corps must be licensed to practice medicine or surgery in a U.S. state, territory, commonwealth, possession, or in the District of Columbia, as required by BUMEDINST 6010.30. (Credentialing and Privileging Program).
Professional Qualifications Review
The professional review board (PRB) of the Bureau of Medicine and Surgery (BUMED) will analyze all applicants’ credentials and professional qualifications.
Prior to submitting an accession package for evaluation by the PRB, the Medical Corps program manager, Commander, Navy Recruiting Command (CNRC), should have the applicant’s credentials validated by the Centralized Credentialing and Privileging Directorate in Jacksonville, Florida.
Medical Corps Service Obligation
Active Duty
From the date of appointment, there is a three-year Active-Duty commitment.
The remaining service time, up to a total of eight years, may be spent in a ready reserve condition.
The receipt of special pay and bonuses, education obligations, and minimum activity tour requirements as a result of being admitted to the Navy as an Active Duty officer may result in an extension of the aforementioned obligation term.
Reserves
Medical Corps Reserve Component selectees will be required to serve an eight-year ready reserve obligation, with the first three years as a Selected Reserve.
The commitment takes effect upon commissioning.
The receipt of a special compensation, bonus, or education requirement may cause the aforementioned obligation term to be extended.
More Information
If you wish more information with regard to becoming a Navy Medical Corps Officer, the next logical step is to contact your local Navy Officer Recruiter.
People also read the Medical Service Corps program.
Hope you find this helpful in your career planning.


